Turkish surgeon Ogün Erşen told an undercover BBC reporter she could qualify for gastric sleeve surgery if she ate “some snacks”.
This video can not be played
To play this video you need to enable JavaScript in your browser.
A Turkish doctor selling weight-loss “holidays” abroad told an undercover BBC reporter to gain weight so she could have gastric sleeve surgery.
Dr Ogün Erşen told the reporter to “eat some snacks” so she could increase her body mass index (BMI) to qualify for his weight loss surgery.
The BBC reporter had a BMI of 24.4, which is within the healthy weight range.
“You must eat, eat. Eat something and reach 30,” Dr Ersen said.
The reporter gave the weight-loss clinic information which would have meant her BMI was 29 but she was not weighed and no medical checks were carried out during her consultation.
Instead, Dr Erşen offered to book her in for surgery in three months’ time and told her to try to put on weight.
A health expert told the BBC it was completely unethical to push a patient to gain weight to hit the threshold for surgery.
He stressed the risks of this irreversible surgery and said it should not be done if it is not needed.
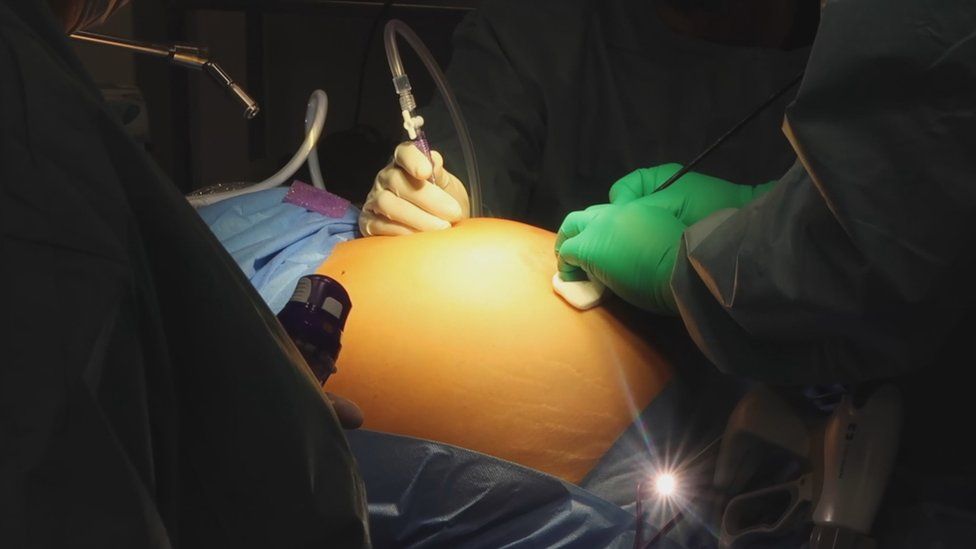
Image source, Cosmedacare
Referrals to weight management services in Scotland are up 96% compared to pre-pandemic levels and waiting lists for bariatric surgery on the NHS can exceed four years in some areas.
The price to have it done privately in the UK is between £10,000 and £15,000 but it can cost as little as £2,000 to book weight-loss surgery in Turkey.
However, a BBC Disclosure investigation has uncovered the unethical practices used by some companies offering cheap weight-loss “holidays” abroad.
Ekol Hospitals is one of the many Turkish companies targeting British customers. It regularly holds sales days in cities across the UK.
Undercover filming at a sales day in Glasgow revealed Ekol accepting patients whose BMI did not meet the criteria for bariatric surgery.
BMI is based on a person’s height and weight and it is one of the main factors when assessing for bariatric surgery.
A patient with a BMI of less than 40, and no severe co-morbidities relating to obesity, would typically be rejected for weight-loss surgery in the UK.
Under the international IFSO guidelines the threshold is lower, at 35.

What is bariatric surgery?
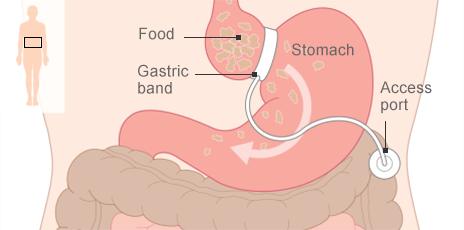
Bariatric surgery, also known as weight-loss surgery, is used by the NHS as a last resort to treat people who are dangerously obese (having a body mass index of 40 or above or 35 plus other obesity-related health conditions).
Patients must have tried and failed to achieve clinically-beneficial weight loss by all other appropriate non-surgical methods and be fit for surgery.
The two most common types of weight loss surgery are:
- Sleeve gastrectomy or gastric bypass, where some of the stomach is removed or the digestive system is re-routed past most of the stomach
- Gastric band, where a band is used to reduce the size of the stomach so a smaller amount of food is required to make someone feel full

At the Ekol sales day, two undercover journalists falsely presented medical information which should have ruled them out
They said their BMIs were 29 and 33 – and one cited depression, all of which should have raised red flags with the consultant.
An Ekol sales rep also encouraged the reporter to eat more and return for surgery at a later date.
The sales rep said: “I yo-yo dieted my whole life, for 30 years, and I got my sleeve two years ago.”
She added: “Do you look into more traditional ways, and risk that yo-yo? Or do you just let it go for a few months and eat like a pig? High fat, high calorie, high everything.”
In a statement, Ekol Hospitals said: “We completely refute the suggestion that our hospital accepts patients for surgeries who do not meet international guidelines or criteria.
“Whilst at the hospital, a full and extensive health check is completed.”
When later asked for a response, the sales rep said: “It is unfortunate that our health care, NHS or private, is unable to cope with the obesity epidemic in our country, ideally every person would have access to the health care they need but that is not the case.”
Dr Erşen denied he made the comments encouraging a patient to gain weight.

Omar Khan, a consultant bariatric surgeon and chair of the National Bariatric Surgery Registry, described the consultation as “utterly indefensible”.
He said: “I have major concerns. It seems that he’s almost pushing the patient to hit the target so that they can do the surgery and that’s completely unethical.
“There’s no surgery which is risk free. What we have to do is balance those risks against potential benefits of weight loss surgery.
“If you take someone who is thin, there’s no point in giving them weight loss surgery, because they’ll take all of the risks of surgery, but none of the benefits.”
Gill Baird, who runs a cosmetic surgery business in Glasgow, says she regularly turns people away for weight-loss surgery because they do not meet the criteria.

She said: “We check for stones in your pockets when you come to the scales.
“We’ve had patients come in with anoraks on and you’ll find that they’ve got weights in their pockets trying to make themselves heavier. It happens quite a lot.
“They do it because they’re desperate, and I can understand that. But they’re not understanding the risks that they’re taking with their health.”
For some British, patients the consequences of going abroad have been fatal.
“Unfortunately, we recently had a situation with a patient from the UK who had inquired with us about a particular procedure,” Ms Baird said.
“She didn’t meet the criteria. We had advised her of that and she told me on the phone that she was going to see a provider who was based abroad the very next day.
“Unfortunately a few weeks later it was in the headlines that she’d sadly passed away as a result of that surgery abroad, which was difficult to process.”