Surgeons left frustrated as hospitals struggle to return routine services to full strength.
 Image source, Getty Images
Image source, Getty ImagesThe push to tackle the hospital backlog is being undermined by the struggle to get services back to full strength.
A BBC analysis shows the expected surge in new patients has not yet happened.
Instead, the waiting list in England is growing because the NHS is carrying out fewer operations and treatments than it was before Covid, despite a government push to boost capacity.
Surgeons said it was really frustrating as operating theatres were not being used due to a lack of beds and staff.
“It’s tough on patients and tough on staff who want to get on and treat patients,” said Tim Mitchell, vice-president of the Royal College of Surgeons of England.
“Without treatment, the health of patients can deteriorate.
“Not only do we need to get back to where we were before the pandemic, we need to do more if we are going to tackle the backlog.”
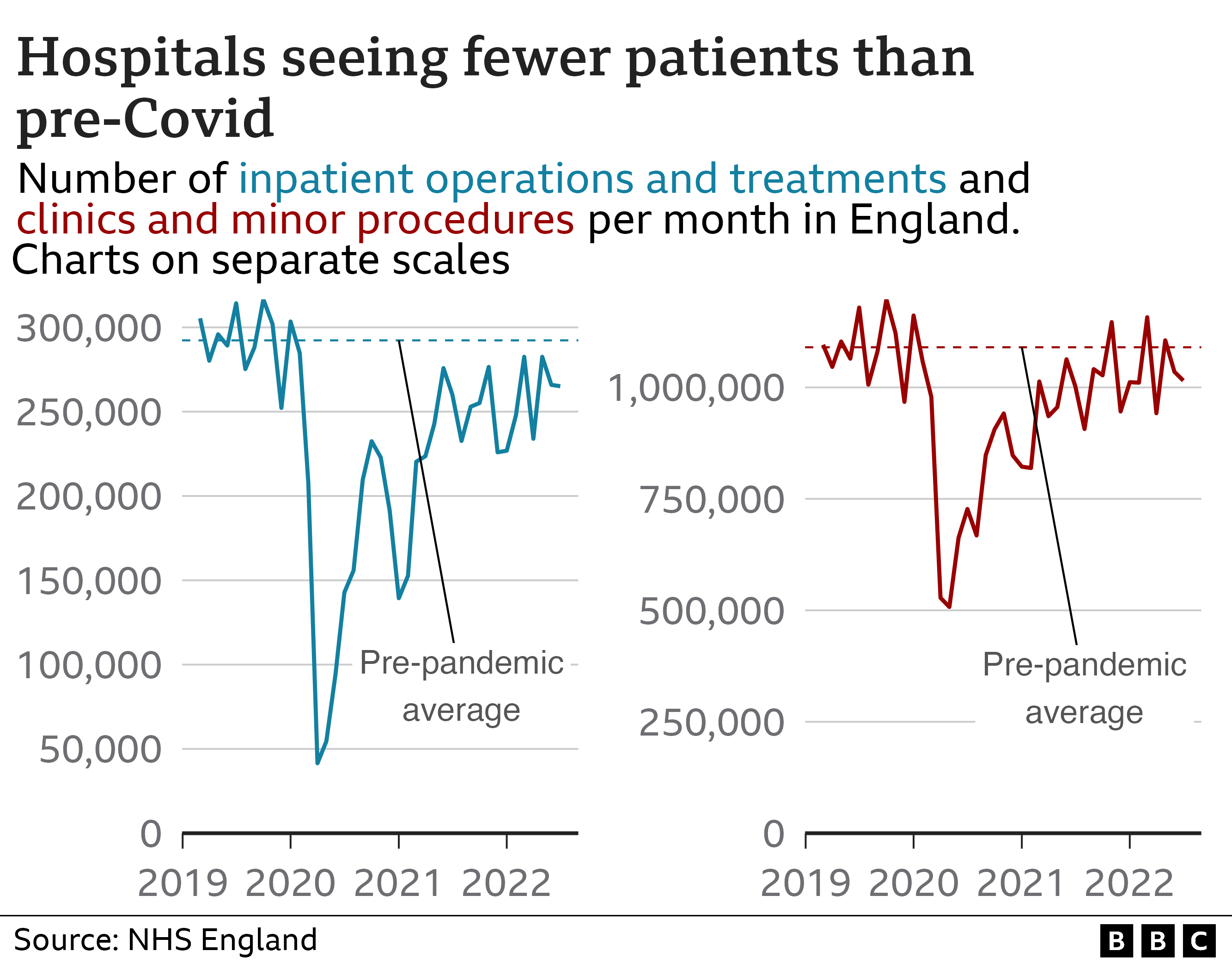
NHS England data shows that in the past year an average of nearly 254,000 inpatient treatments, including hip and knee replacements, have been performed each month.
That is 13% lower than the year before the pandemic.
Outpatient clinics, which include minor procedures, tests and assessments, are down by 6% to just over one million a month on average.
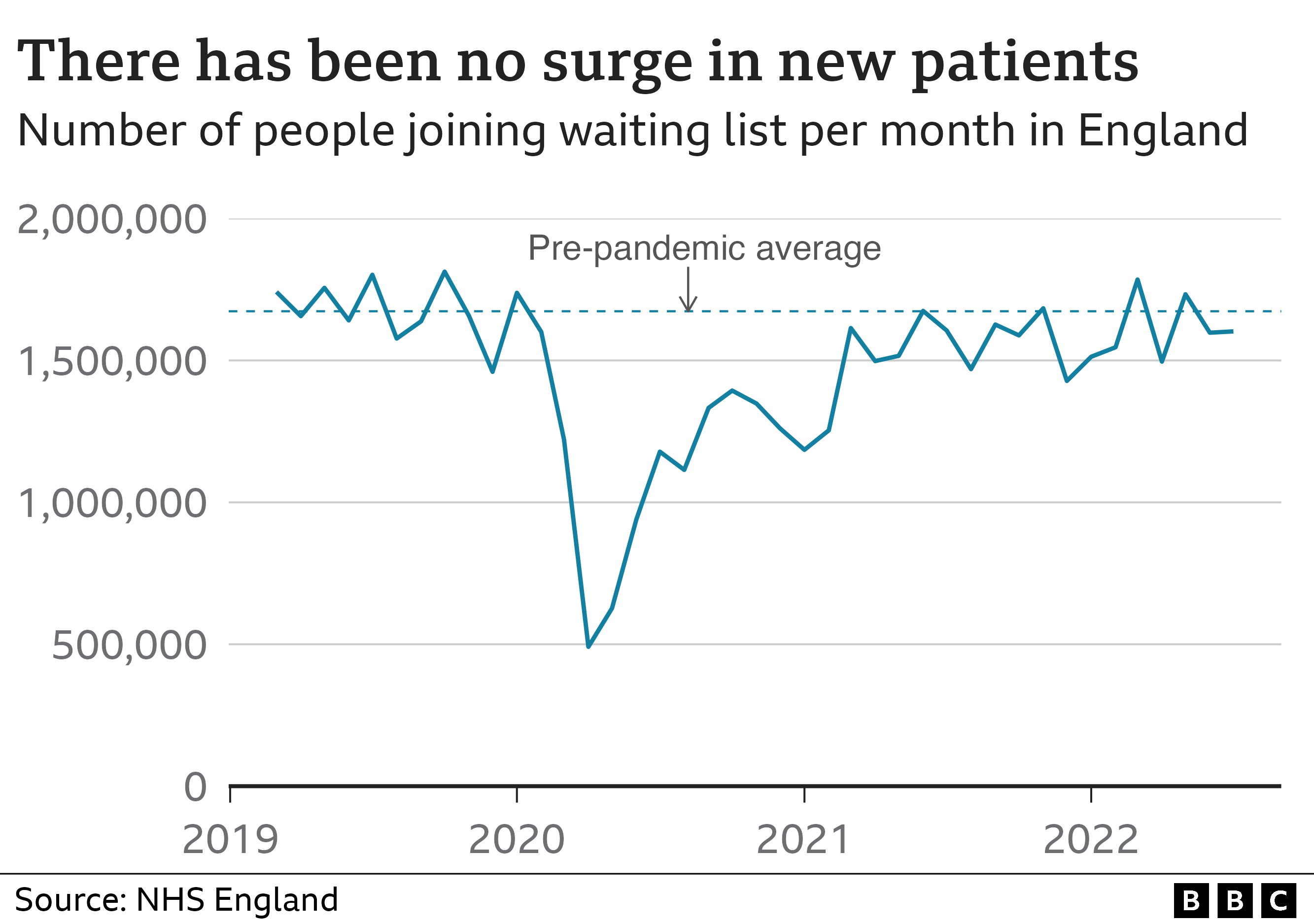
The struggle to return services to full strength is why the backlog is growing, because the number of new referrals for treatment has not actually gone up above its average before the start of the pandemic.
This has surprised many in the health service, because it was always expected there would be a lot of extra demand at this point given how many people did not come forward when Covid first hit.
Mr Mitchell said there was likely to be a lot of hidden demand out there with people either still staying away or struggling to make it on to the waiting list because of pressure on GP services.

‘Wait for op affecting my physical and mental health’

Marcus Mansukhani has been waiting for a hernia operation since late 2018.
Surgery initially had to be put off because he had high blood pressure and then the pandemic hit, delaying his treatment even further.
He then needed to have his gall bladder removed and that took place two months ago.
In the meantime, his hernia has grown to 4.7in (12cm) in size. It is so big, he is struggling to walk.
Ms Mansukhani, 47, from Suffolk, said: “It is very frustrating.
“I’m not walking as much as I would like because it is painful. And it is noticeable when I go out in public, so I’ve been keeping myself to myself.
“Something like this really affects both your physical and mental health.”

Mr Mitchell said there was a range of factors which meant hospitals continued to have to run routine services at below capacity.
This included continued disruption by Covid, which was causing both increased illness among staff and more beds being taken up by sick patients, and delays freeing up beds, because some patients cannot be discharged as they cannot access necessary care in the community.
The NHS in England has been set a target of carrying out 30% more treatments by 2024.
To help, a network of community diagnostic centres and surgical hubs away from hospitals are being established.
But Mr Mitchell warned there was still a lack of staff in places to make the most of this investment – he said there were particular problems with theatre nurses and anaesthetists.
And he said this was a UK-wide issue, pointing out the situation in Wales and Northern Ireland was particularly bad.
‘Progress is being made’
Ministers have warned it may be spring 2024 before the backlog starts to fall in England. Currently nearly seven million people are waiting for treatment.
Saffron Cordery, of NHS Providers, which represents hospitals, accepted there was “still a long way to go”.
But she added: “Trusts are working incredibly hard to recover ground lost in tackling care backlogs.”
Siva Anandaciva, of the King’s Fund think tank, said the problems were “fundamentally” linked to a lack of resources.
“If you look at other countries, the NHS has fewer doctors, nurses and hospital beds.
“Even the most efficient system in the world can only get through so much work if it hasn’t got the fundamental resources it needs.”
But an NHS England spokeswoman said the health service was “making significant progress”, having virtually eliminated two-year waits and making inroads on the number of people waiting 18 months.
She added: “There is now considerable investment in surgical hubs and diagnostic centres that will help to protect elective treatments from wider pressures, especially in future years, and increasing use of technology like robotic surgery and dedicated day case units, which help increase the amount of elective procedures that can be carried out.”
Data visualisation by Will Dahlgreen