As the health safety watchdog warns on ambulance delays, the BBC investigates the case of 94-year-old Ken Shadbolt.
 Image source, Family photo
Image source, Family photoDelays unloading ambulances at busy hospitals are causing serious harm to patients, a safety watchdog is warning.
The Healthcare Safety Investigation Branch has been investigating how the long waits are delaying 999 emergency response times across England.
Kenneth Shadbolt, 94, waited more than five hours for an ambulance after a bad fall – an accident that proved fatal.
Logs show that in his final 999 call he asked: “Can you please tell them to hurry up or I shall be dead.”
The BBC has been given permission from the coroner to view detailed evidence into his recent death.

Ken Shadbolt had been in good shape for his age.
A retired factory worker and carpenter, he lived alone in a semi-detached house in the market town of Chipping Camden in the Cotswolds, and could often be spotted cycling around the local housing estate on his electric trike.
On the night of Wednesday, 23 March 2022, he called one of his five sons for a chat before turning in for the night.
Just before 03:00, he got out of bed to go the bathroom and fell, hitting a wardrobe before collapsing on the floor.
He had hurt his hip – how badly he didn’t know – and couldn’t get up. He could reach his mobile on his bedside, though, and dialled 999 for help.
The BBC has seen transcripts of the three separate phone calls he made to South Western Ambulance Service that night.

Image source, Family photo
The first call: 02:58
The first was short and factual, covering the basic details of his injury.
He seemed calm and lucid but made clear he was in pain and needed an ambulance.
He was told by the call handler not to try to move unless he felt in danger and assured that help was “being arranged”.
“How long will it be?” he asked.
“I don’t know, unfortunately, [but] we will try to get someone there as soon as we can,” came the reply.
He then spoke to one of his sons who offered to drive up that night from the other side of the country.
Ken said he thought an ambulance was on the way, and not to worry.
Internal call logs seen by the BBC show that at this point Ken was triaged as a category two emergency, meaning paramedics should arrive in 18 minutes, on average.
That didn’t happen.

Image source, Family photo
The second call: 03:13
About 15 minutes later, he called 999 for a second time.
It was clear by now that he was starting to worry.
He said he couldn’t move his right leg and talked about an injury to his shoulder as he’d hit the floor. He was worried about his mobile phone, saying the battery “won’t last forever”.
“When I rang up 999 I thought I would get some treatment straight away,” he told the next person on the line.
“It is still down as an emergency response,” the call handler replied. “We are extremely busy at the moment but we are working on getting that help to you as quickly as we possibly can, ok?”
An internal ambulance service log seen by the BBC shows that South Western Ambulance Service was indeed busy that night.
It talks about “high demand” in the Gloucester area, with more than 60 patients waiting for help, some for more than eight hours.
But something else was going on at the same time.
The local A&E was very full, so paramedics arriving outside the emergency department were unable to unload their sick patients straight away.
The ambulance service log warns there were “long delays with unloading at GRH [Gloucestershire Royal Hospital]” that night.
Data seen by the BBC shows that 75% of ambulances were delayed for at least half an hour at Gloucester or its sister hospital in Cheltenham on 24 March, with 54% having to wait for more than an hour.
That handover should be completed in under 15 minutes.
If paramedics are queuing outside A&E, then they are not able to get back on the road and quickly pick up the next patient who needs help.
A doctor’s report into Ken’s case specifically refers to “a lack of ambulances available” that night.

The third call: 04:12
Another hour passed before he made his third and final call to 999.
It was clear now that he was in serious pain. He felt “terrible sick” and said his “breathing is going too”.
“I need an ambulance because I’m going to fade away quite quickly,” he said.
The same reply came back: “The ambulance service is just under a lot of pressure at the moment… we are doing our best.
“I appreciate that you’ve been stuck for quite some time, Ken… we’ve not forgotten about you at all.”
Later in the call he said he was cold and could not reach his duvet. He’d already tried phoning one of his neighbours but could not get through, and said they “might be away”.
He was told by the 999 call handler to “try to stay still”.
“Can you please tell them to hurry up or I shall be dead,” he said.
“Send me the undertaker, that would be the best bet.”
He put the phone down for the last time.

‘Non-survivable’
An ambulance finally got to Kenneth Shadbolt’s house at 08:10 that morning, four hours after that final call.
By then one of his sons had contacted a neighbour, who found him unconscious on his bedroom floor.
He arrived at Gloucestershire Royal Hospital at 09:59, and was handed over to the trauma team.
A doctor phoned the family and told them to come straight away, as by then his injuries were not survivable.
Ken died at 14:21 that afternoon, with the cause of death given as a “very large subdural haematoma” or bleed on the brain.
His son Jerry Shadbolt said: “The doctors were saying his injuries were non-survivable but would they have been non-survivable if he’d arrived at hospital four hours earlier? I’d like an answer to that question.
“He was on his own and he knew he was on his own. He must have felt abandoned and alone on his bedroom floor. That’s the most troubling part of it for me.”
‘Unacceptable’
Jenny Winslade, executive director of quality and clinical care for the South Western Ambulance Service NHS Foundation Trust, offered her “sincere condolences” to the family and friends of Mr Shadbolt.
She said delays handing over patients to A&E, and busy hospitals, meant it was “taking us too long to get an ambulance to patients”.
“This is a risk which we recognise is unacceptable,” she said.
“We continue to work on a daily basis with our partners to ensure our crews can get back out on the road as quickly as possible, to respond to other 999 calls.”
Prof Mark Pietroni, medical director and acting chief executive of Gloucestershire Hospitals NHS Foundation Trust, said local and national health systems were “under intense pressure” and continued to face significant challenges “in response to unrelenting demand”.
The trust said that, currently, 240 hospital patients – out of a total of 837 beds for patients – were waiting for support to go home or be moved to other locations in the community.
The national picture
Doctors and paramedics have become increasingly concerned about long ambulance wait times across the UK this year.
In England as a whole, the average response for a category two emergency, such as a heart attack or stroke, has risen to more than 51 minutes – almost three times longer than the 18-minute target.
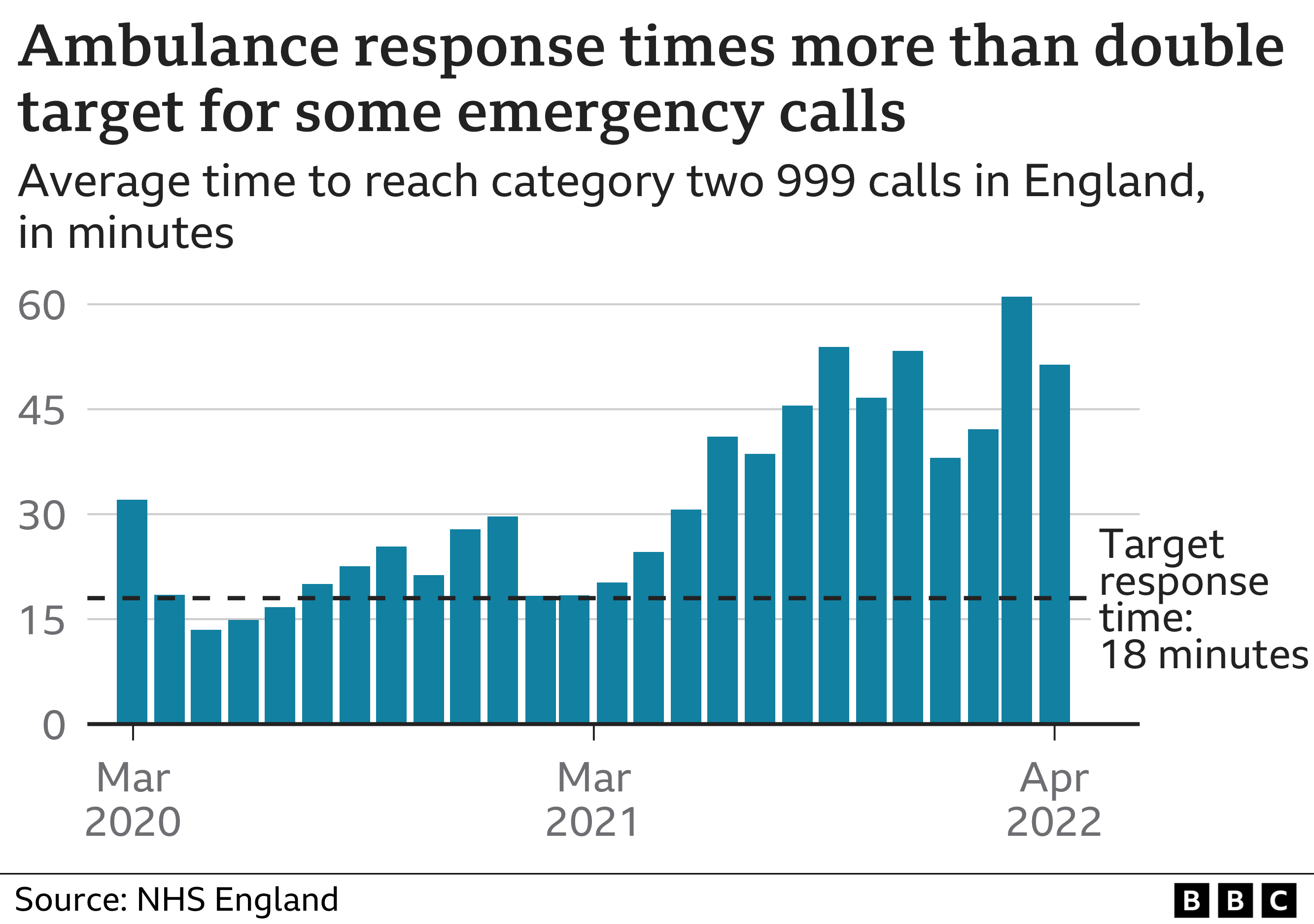
Last month, Dr Katherine Henderson, an A&E consultant and president of the Royal College of Emergency Medicine, described the situation as “more serious than we’ve ever seen it”.
She said the problem is often caused by delays discharging patients from hospital wards into a care setting, which then creates a bottleneck in A&E, leaving no space for new patients arriving by ambulance.
The BBC has spoken to people who have spent hours waiting outside emergency departments this year, sometimes transferred between different ambulance vehicles because there is no room to treat them in the hospital itself.
The Healthcare Safety Investigation Branch (HSIB) says the delays are causing harm to patients, including some deaths.
Its final report will be published later this year, but the interim findings – released on Thursday – show that staff who have witnessed harm to patients and their families are traumatised.
“Harm is happening on a daily basis,” said the HSIB’s national investigator Neil Alexander.
He referred to patients deteriorating in ambulances while waiting for treatment in emergency departments, and patients getting infections in hospital because they were staying there too long.
“And we are no longer using the word ‘risk’ in this investigation, because risk is being realised and is now harm,” Mr Alexander said.
The government said it would carefully consider the HSIB’s report and would “respond in due course”.
“The NHS has allocated £150m of additional funding to address pressures on ambulance services, with the number of ambulance and support staff increasing by almost 40% since February 2010,” said a spokeswoman for the Department of Health and Social Care.
“We have also established a national taskforce to identify ways to reduce delayed discharges and ensure patients are only in hospital for as long as they need to be.”
You can follow Jim on Twitter.